
Spina Bifida —
The Split Spine.
Spina Bifida is a birth defect caused by the incomplete closure of one or more vertebral arches of the spine during embryonic development — resulting in malformations of the spinal cord that range from hidden to life-threatening.
Bifida

Every Child Deserves the Best Chance
FFF supports children with Spina Bifida across Nigeria
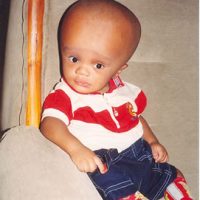
FFF's Work with Spina Bifida
Nigeria · Awareness · Surgery · Continence · Inclusion
Tube
Defect
A Gap in the Spine — Present from Birth
Spina Bifida comes from the Latin for "split spine." These are birth defects caused by an incomplete closure of one or more vertebral arches of the spine, resulting in malformations of the spinal cord. The fault in the development of the spinal cord and surrounding bones (vertebrae) leaves a gap or split in the spine.
Depending on the type, Spina Bifida can be potentially life-threatening or result in severe disabilities. It occurs in the first month of pregnancy — often before a woman even knows she is pregnant — making preconception care and folic acid supplementation critically important.
The Three Types of Spina Bifida
Spina Bifida presents in three distinct forms. Each varies significantly in severity, visibility, and impact on the person's life — from entirely hidden to visibly life-altering.
Spina Bifida Occulta
In occulta, there is no opening of the back, but the outer part of some vertebrae are not completely closed. The split in the vertebrae is so small that the spinal cord does not protrude. The skin at the site of the lesion may be normal, or may have some hair growing from it, a dimple, or a birthmark.
Many people with this form do not know they have it, or symptoms do not appear until later in life. However, the degree of disability can still vary and be very severe depending on the location of the lesion.
Spina Bifida Cystica
In this most serious form, the meningeal membranes covering the spinal cord — and part of the spinal cord itself — protrude through a cleft, forming a clearly visible sac or cyst containing tissue, cerebrospinal fluid, nerves, and part of the spinal cord.
The spinal cord is damaged or not properly developed. There is usually some degree of paralysis and loss of sensation below the damaged vertebrae. The amount of disability depends on where the Spina Bifida is and the amount of nerve damage involved.
In approximately 90% of people with myelomeningocele, Hydrocephalus — extra fluid in the brain's ventricles — will also occur.
Meningocele
In this least common form, the outer part of some vertebrae are split and the meninges are pushed out through the opening, appearing as a sac or cyst containing the meninges and cerebrospinal fluid. Crucially, the nerves are not usually badly damaged and are able to function.
There is often little disability present, and there are usually no negative long-term effects — although problems have been known to arise in some cases.
Causes & Prevention
What Causes Spina Bifida?
Spina Bifida is caused by the failure of the neural tube to close during embryonic development. Normally, closure of the neural tube occurs around the 30th day after fertilisation. If something interferes and the tube fails to close properly, a neural tube defect results.
Spina Bifida occurs in the first month of pregnancy — often before the woman knows she is pregnant. The incidence varies across the world depending on geographic region, season at conception, gender of affected infants, ethnicity, socioeconomic status, maternal age, and parity.
Neural tube defects include anencephaly, encephalocele, and Spina Bifida. Declining prevalence in developed nations is attributed to early diagnosis, selective termination, genetic counselling, and nutritional supplementation.
Prevention
There is no single cause of Spina Bifida and no known way to prevent it entirely. However, research has shown that appropriate intake of folic acid — a B vitamin — before and during early pregnancy can prevent 50–70% of neural tube defects.
It is recommended for all women of childbearing age and women planning to become pregnant to take at least 0.4 mg/day of folic acid from at least one month before conception, continued through the first 12 weeks of pregnancy.
Women who have already had a baby with Spina Bifida, or who are taking anticonvulsant medication, should take a higher dose of 4–5 mg/day. How or why folic acid helps to prevent Spina Bifida is not yet fully understood.
Folic Acid: The Most Powerful Preventive Tool
Folic acid (Vitamin B9) supports proper neural tube closure. Supplementation before and during pregnancy is the single most effective preventive measure available. Sources include whole grains, fortified breakfast cereals, dried beans, leaf vegetables, and fruits.
for all women of childbearing age
births or anticonvulsant use
Living with Spina Bifida
Spina Bifida results in varying degrees of physical and developmental challenges depending on the severity and location of the lesion on the spine. Most babies born with the condition will require multiple surgeries and long-term, intensive therapeutic support.
Varying degrees of paralysis and loss of sensation below the damaged vertebrae, depending on the location and severity of the lesion.
Hydrocephalus — excess fluid in the brain's ventricles — occurs in up to 90% of children with Myelomeningocele (MMC), requiring shunt surgery.
Bladder and bowel incontinence due to neuropathic damage, which requires ongoing management through catheterisation, medication, and bowel programmes.
Spine and limb problems including hip dislocations, foot deformities, and scoliosis, which may require surgical intervention or adaptive equipment.
Loss of skin sensation in lower limbs and around the sacral area, increasing risk of pressure sores and skin breakdown.
In very rare cases, cognitive difficulties may also present — though most individuals with Spina Bifida have normal or near-normal cognitive function.
There is currently no cure for Spina Bifida. Treatment requires a lifelong, multidisciplinary approach beginning at or before birth.
Treatment Pathway
Management begins with surgical repair of the spine and continues with a lifetime of multidisciplinary interventions to prevent deterioration and maximise quality of life.
Spinal Closure Surgery
Surgical closure of the spinal opening is performed soon after birth to minimise infection risk and prevent further nerve damage.
Shunt Surgery for Hydrocephalus
A VP shunt is inserted to drain excess cerebrospinal fluid from the brain's ventricles, preventing dangerous pressure build-up.
Continence Management
Bladder and bowel function is managed through catheterisation, bowel washouts, medication (e.g. Oxybutynin), and ongoing monitoring to protect kidney health.
Mobility & Orthopaedic Support
Braces, orthotics, wheelchairs, and physiotherapy help children achieve maximum mobility and prevent secondary complications.
Developmental Therapy
Long-term occupational therapy, speech therapy, and psychosocial support encourage development and promote full participation in education and community life.
In developing countries like Nigeria, late presentation is the norm — driven by cultural and religious beliefs and inadequate healthcare personnel. Aggressively pursuing strategies to reduce incidence and improve access to early care is essential.
How FFF Supports Children with Spina Bifida
Continence Management (SLIF)
FFF's flagship SLIF Project trains health workers and establishes continence clinics across Nigeria — providing free CIC kits, bowel management, urodynamic monitoring, and Oxybutynin to children with Spina Bifida in 9 teaching hospitals.
View SLIF Project →Surgery Sponsorship
FFF sponsors surgical procedures for indigent children with Spina Bifida — including spinal closure and shunt surgery — subject to donor funding availability, through the Medical Support Programme.
Medical Support →Support Groups
FFF facilitates peer support groups for families and children affected by Spina Bifida — providing psychosocial support, practical guidance on daily care, and community to reduce isolation.
Support Groups →Awareness & Advocacy
Through annual SBH Day events, media campaigns, school sensitisation, and policy engagement, FFF raises awareness about Spina Bifida, breaks down stigma, and advocates for better government funding of SBH services.
SBH Day →Inclusive Education
FFF works to ensure children with Spina Bifida are enrolled and supported in Lagos State's public inclusive schools — addressing the chronic exclusion of children with disabilities from mainstream education.
Inclusive Education →Counselling & Referrals
FFF provides counselling for families navigating new diagnoses and connects them with the right specialist hospitals, rehabilitation services, and social support networks across Nigeria.
Counselling & Referrals →Support Children with Spina Bifida in Nigeria.
Your donation to FFF directly funds continence care, surgery sponsorship, inclusive education, and awareness campaigns for children and families living with Spina Bifida across Nigeria.
Trusted Partners & Members




